
Peripheral artery disease and neuropathy make it simpler to develop infections and ulcers. As a result, ischemia, a dark tissue that is one of the early warning symptoms of gangrene, may emerge. The skin tissues surrounding a diabetic foot ulcer that is not immediately treated risk losing blood and oxygen due to lack of supply. The term used to describe when body tissue dies due to a bacterial infection or a reduction in blood supply. As the bones age, they become brittle and begin to fracture or dislocate in response to light pressures, like walking. They might potentially result in Charcot foot. Deformities in the feet can develop from weakening of the muscles and bones of the feet caused by long-term uncontrolled diabetes and diabetic foot infections. When the body’s immune system overreacts to an infection and starts to harm tissues and organs, this illness could be fatal. Sepsis.Sepsis may result from an infection that has spread far enough to infiltrate the bloodstream.A painful collection of pus beneath the skin’s surface, may develop from an infected diabetic foot ulcer. Amputation risk increases if the infection travels from the incision to the bone. Skin infections from diabetic foot ulcers can cause swelling around the wound site, foul-smelling discharge, fever, and chills. 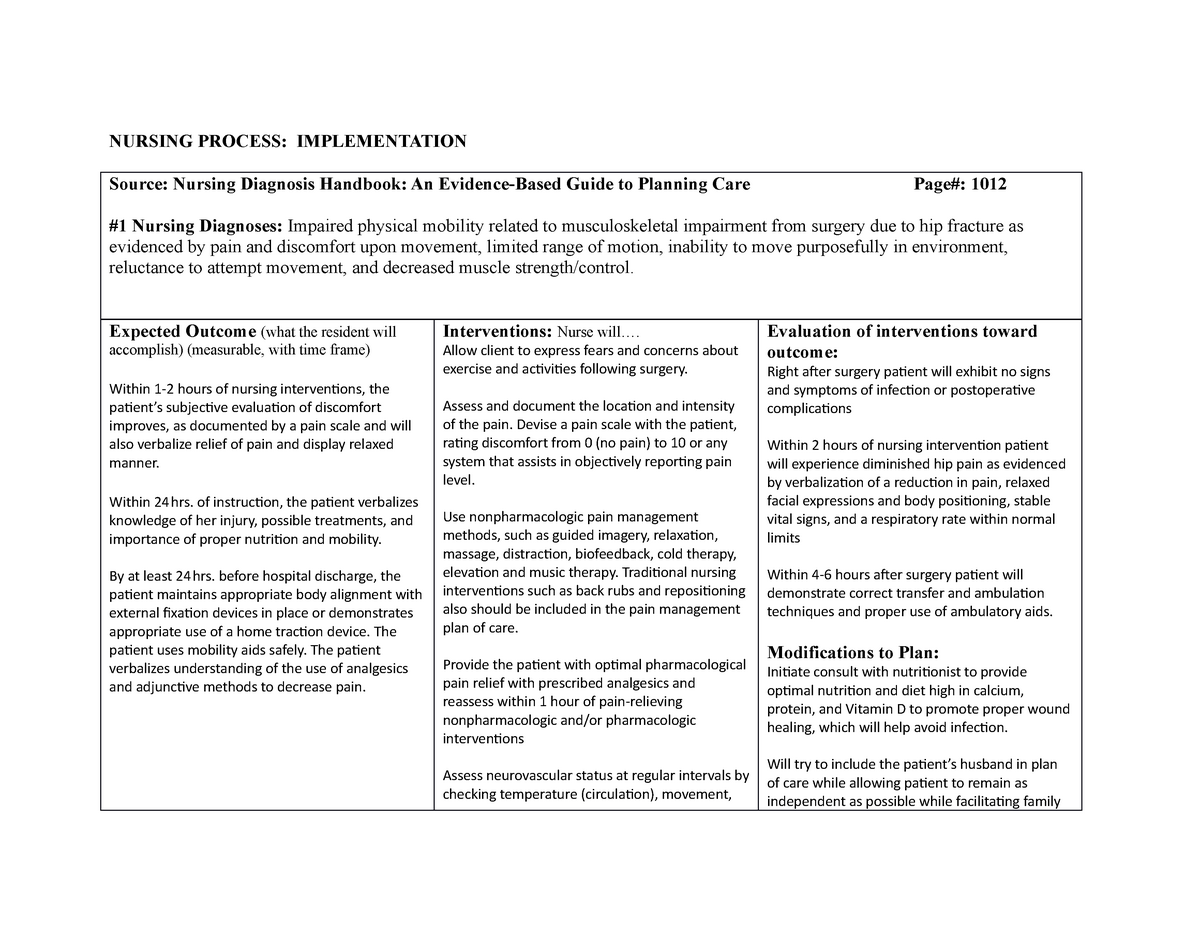 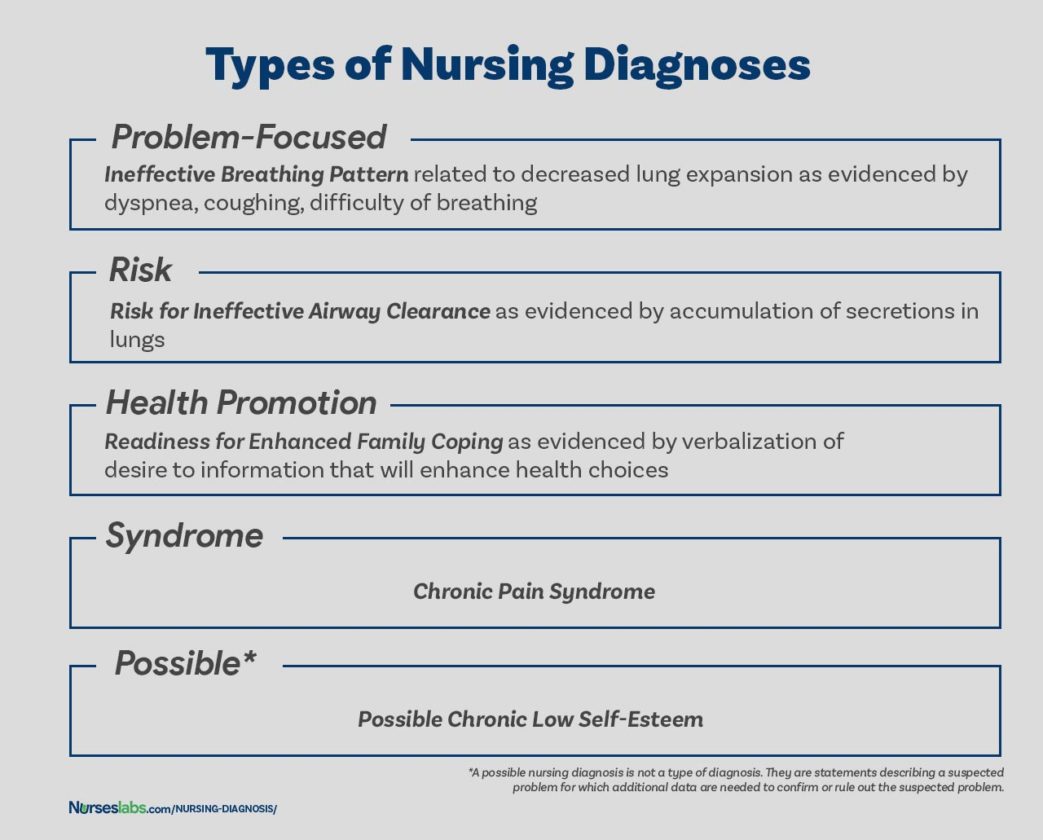
The emergence of this illness raises the possibility of getting a diabetic foot ulcer. When bones, joints, and the soft tissue of the foot and ankle become inflamed as a result of neuropathy, a Charcot joint forms. These circumstances have a detrimental effect on healing and may lead to the persistence of lesions that may develop into ulcers. Smoking has been linked to additional comorbid conditions such arterial and vascular disease and chronic obstructive pulmonary disease, as well as the onset of foot ulcers and gangrene. Additionally, the majority of them are between the ages of 40 and 70. Male individuals with diabetes are more likely than female patients to develop foot ulcers. This illness can be managed with a mix of oral medications and insulin treatment. Hypertension.More than half of diabetic people who develop foot ulcers also have hypertension.Ulcers typically develop in places that are prone to recurrent shear or stress, particularly if the calluses are hemorrhagic. In order to prevent foot ulcers in diabetic individuals, it is essential to recognize new lesions. The likelihood of infection and necrosis can rise as a result of the resultant ischemia. Insufficient blood flow is caused by peripheral vascular disease, especially in the lower limbs. The occurrence of any type of diabetic neuropathy, particularly polyneuropathy, which is characterized by altered vibration, position, temperature sensations, numbness or pain, and other symptoms, increases the risk of developing diabetic foot ulcers. Diabetic patients with flat foot impose uneven tension on the foot which causes tissue inflammation in high-risk foot areas. Obesity.Obese people with diabetes may be especially at risk for developing peripheral neuropathy, peripheral arterial disease, and becoming unable to care for themselves.Drainage from the affected area and occasionally a pronounced bulge that is not necessarily painful are indications of an ulcer. Nerve damage can cause tingling and pain, it also causes painless ulcer-causing sores and lowers the sensitivity to foot pain. The long-term impact of nerve damage is a lack of sensation in the feet. People with type 2 diabetes and other illnesses frequently struggle to combat ulcer-related infections. Blood sugar control is essential because high glucose levels might hinder the healing of an infected foot ulcer. High blood sugar level or hyperglycemia.It causes an inefficient blood flow to the feet and ulcers may be more difficult to heal if there is poor circulation. That reduces blood flow, which makes it more difficult for cuts and sores to heal particularly in the hands, feet, and limbs. The nerves and blood vessels can become damaged by excessive blood sugar levels. any changes to the toenails and skin which include cuts, blisters, calluses or sores.eschar or black tissue surrounding the ulcer.foul-smelling odor from one or both feet.Signs and Symptoms of Diabetic Foot Ulcer
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
